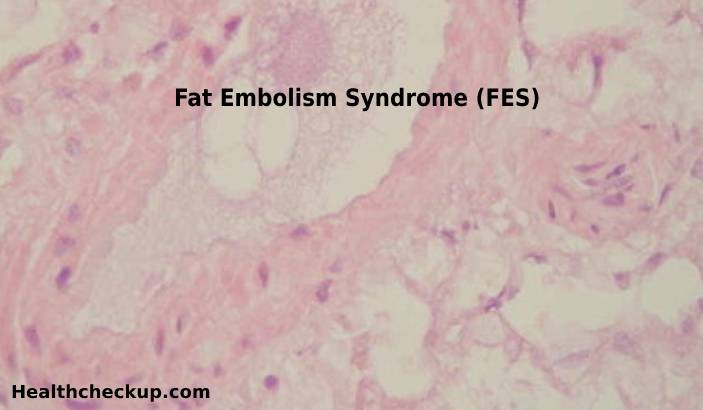
Fat Embolism Syndrome (FES) is an indistinct clinical condition manifested by the presence of systemic symptoms caused due to fat embolism. Fat globules or particles that travel through the blood circulation are called Fat Emboli. Fat embolism is a process by which the fat emboli passes through the bloodstream and lodges in the blood vessel causing blockage of blood flow to that area. [1]
What is Fat Embolism Syndrome?
The block within the blood vessels (capillary bed) caused by fat emboli results in tissue damage and also systemic inflammatory reactions causing a triad of respiratory, neurological and dermatological dysfunction known as Fat embolism syndrome (FES). [2]
Who discovered FES?
In 1862, Zenker first described this syndrome in a patient with thoracoabdominal crush injury and suggested that the fat originated from the lacerated stomach. In 1873, Von
Bergmann clinically discovered FES for the first time in a patient with a fracture. [3]
What is the Incidence of FES?
- Traumatic fat embolism occurs in 90 % of individuals with severe skeletal injuries [4].
In the orthopaedic and trauma literature, the incidence of FES has ranged from <1% to >30% of cases. It is estimated to occur in 3-4% of patients with a long bone fracture. The incidence increased to 0.54% in isolated femoral fractures and 1.29% if multiple fractures including the femur were present. [5] [6] - Gurd reported the incidence of FES as 19% in a group of trauma patients.[7].
Approximately 3 to 4% of patients develop the classical triad of FES. Most go undetected due to the mild symptoms. [8] - FES is associated with a 1-2 percent mortality rate [9]
What are the causes of FES?
FES mostly occurs secondary to orthopaedic trauma; Fat embolism subsequently becomes FES and can be categorized into Traumatic and Non-traumatic causes;[10] [11] [12]
- Traumatic Causes
- Fracture of the long bones of
− Femur
− Pelvis− Tibia - After Orthopedic surgeries – Post-operatively
− Pelvic
− Knee arthroplasty and
− Intramedullary nailing and reaming - Multiple traumatic injuries
- Other rare traumatic causes
− Massive soft tissue injury
− Thoracoabdominal crush injury
− Prolonged cardiopulmonary resuscitation
− Bone marrow harvest/transplantation
− Bone marrow biopsy
− Severe burn (> 50 %)
− Median sternotomy
- Fracture of the long bones of
- Non-traumatic causesThese are usually very rare causes and they include the following:
- Sickle cell disease
- Thalassemia
- Acute Pancreatitis
- Decompression sickness
- Fatty liver
- Hemoglobinopathies
- Corticosteroid therapy
- Lymphography
- Osteomyelitis
- Liposuction
- Parenteral feeding with lipid infusion (Fat emulsion infusion)
Who is at risk of developing FES?
The risk factors for the development of FES include:
- Young people
- Men at a higher risk than women
- Closed fractures
- Multiple fractures, and
- Conservative therapy for long-bone fractures
How does FES develop?
The exact mechanism for the development of FES is not clear. However, two main theories explain the development of FES.
- Mechanical Theory
This theory suggests that the bone marrow contains high content of fat and following a trauma or surgery leads to the release of fat globules into the bloodstream directly obstructing (80%) of the pulmonary and systemic circulation, hence this is called the Mechanical ‘Obstruction’ Theory. Obstruction in the pulmonary capillaries mesh leads to increased lung pressure, oedema, and right-sided heart failure causing severe difficulty in breathing. The fat globules that get access to the systemic circulation make way into the brain, heart, skin and retina affecting them. [14] [15] - Biochemical theory
This theory suggests that a series of hormonal changes are triggered by a traumatic or nontraumatic injury. The lungs respond by secreting tissue lipase to hydrolyse /break down the fat globules, this action leads to the release of high concentrations of glycerol, free fatty acids (FFA) and toxins into the bloodstream. These FFA and toxins migrate into the organs via systemic circulation triggering a cascade of inflammatory reactions leading to multi organ dysfunction. [16]
What are the earliest signs of FES and when are they manifested?
Respiratory problems like dyspnea and acute hypoxemia are usually seen first, followed by neurological dysfunction and petechial skin. Most patients manifest symptoms within 24 to 72 hours after injury. [17] [18]
What are the signs and symptoms?
The signs and symptoms include the general and clinical triad of FES, [17] [18] [19] [20]
- General signs and symptoms include:
− Pain due to the injury
− Generalized weakness
− Fever - Cardiovascular manifestations
− Tachycardia
− Ventricular dysfunction
− Disseminated intravascular coagulation (DIC)
− Thrombocytopenia or Anemia - Pulmonary manifestations− Hypoxemia (96% affected)
− Dyspnea
− Tachypnea
− Acute Respiratory distress syndrome (ARDS) - Neurological abnormalities
− Focal deficits
− Confusion, Delirium or Stupor
− Agitation/restlessness from hypoxia
− Seizures
− Lethargy
− Coma - Skin Problems
− Petechial hemorrhagic rash (conjunctivae, head, neck, anterior thorax, or axillae). - Eye abnormality
− Retinal hemorrhage
What is the classical triad of FES?
The classical Fat embolism syndrome triad includes pulmonary, neurological, and skin abnormalities. [19] [21]
What are the diagnostic Fat Embolism Syndrome criteria?
-
Gurd’s Major and Minor Criteria
It is mostly used for the diagnosis of FES, at least one major and four minor criteria must be present. [6]
Table 1 – Gurd’s CriteriaMajor criteria
- Axillary or subconjunctival petechiae
- Hypoxaemia PaO2 <60 mm Hg; FIO2 = 0.4)
- Central nervous system depression disproportionate to hypoxaemia
- Pulmonary oedema
Minor criteria
- Tachycardia <110 bpm
- Pyrexia <38.5°C
- Emboli present in the retina on fundoscopy
- Fat present in urine
- A sudden inexplicable drop in haematocrit or platelet values
- Increasing ESR
- Fat globules present in the sputum
-
Lindeque’s criteria
Lindeque et.al proposed criteria based on respiratory features alone [22]
Lindeque’s criteria
- Sustained Pao2 <8 kPa
- Sustained PCO2 of >7.3 kPa or a pH <7.3
- Sustained respiratory rate >35 breaths min−1, despite sedation
- Increased work of breathing: dyspnoea, accessory muscle use, tachycardia, and anxiety
-
Schonfeld’s criteria
Schonfeld et al. proposed a measure to diagnose FES; where a score of more than 5 is required to diagnose.[23]
Schonfeld’s criteria
Score
- Petechiae 5
- X-ray chest diffuse infiltrates 4
- Hypoxemia 3
- Fever 1
- Tachycardia 1
- Tachypnea 1
- Confusion 1
List of Laboratory investigations
- Blood picture: may reveal a decrease in hemoglobin, and hematocrit level, and increased lipase and ESR level. Thrombocytopenia, anemia, hypofibrinogenemia, Hypocalcemia and hypoalbuminemia may be evident. [24] [25]
- Urine analysis: the presence of fat globules
- Arterial Blood Gas (ABG) analysis: May reveal hypoxemia (PaO2 < 60 mmHg), with hypocarbia and respiratory alkalosis. [26]
Diagnostic Imaging studies
The imaging studies are said to be very crucial in the early diagnosis of FES and reveal the following: [27] [28] [29]
- Chest X-ray:
− Increasing diffuse bilateral pulmonary infiltrates,
− Pulmonary edema
− Fleck-like pulmonary shadows (‘snow storm’ appearance) - CT (computerized tomography) head:
− Diffuse white-matter petechial hemorrhages consistent with microvascular injury −
Minimal edema - Ventilation/perfusion imaging of the lungs:
− Subsegmental perfusion defects. - <4. Spiral chest CT for pulmonary embolism:
Changes in the parenchymal are evident and consistent with lung contusion, acute lung injury and ARDS - Magnetic resonance imaging (MRI) brain:
− FES lesions present deep in the white matter, brainstem and cerebellum ganglia − Star- field pattern of diffuse, punctate, hyperintense lesions on diffusion-weighted imaging. - 6. Contrast Venography: Diagnostic gold standard of thromboembolism.
Fat Embolism Syndrome Treatment
There is no specific treatment for FES. Immediate management aims at supporting the respiratory function and stabilizing the hemodynamic status of the patient. [30]
Prevention and early diagnosis with prompt management of complications are of utmost importance in saving the life of the patient. The only proven treatment for FES is supportive care of the organ systems that are involved.
Supportive care [2] [16] [25]
a. Continuous monitoring:
− Cardiac Monitoring: Monitor the vitals of the patient continuously, check the CVP level
− Glasgow Coma Scale (GCS): To assess for neurological deterioration, as cerebral edema may lead to rapid deterioration of the patient
− Continuous pulse oximetry monitoring: To detect early desaturation and for immediate supportive management [29]
b. Oxygen Supplementation:
Supplemental oxygen (90%) is required to improve oxygenation.
c. Ventilatory Support:
Intubation may be required if the patient develops ARDS to maintain arterial oxygenation
d. Hemodynamic stabilization:
Albumin and balanced electrolyte solution have been recommended for volume resuscitation to avoid developing shock and restore blood volume
e. Medications:
(Effectiveness of the below-mentioned drugs is still in question) −
Corticosteroid therapy: Used as an anti-inflammatory agent. Some studies have proposed this therapy for FES as it limits free fatty acid levels, stabilises membranes, reduces edema and inhibits complement-mediated leukocyte aggregation.
− Inotropic support with dobutamine: as FES may cause right ventricular failure
DVT prophylaxis: Anticoagulant drugs like heparin or warfarin are commonly used
f. Early stabilization of fractures
Prevention of FES in patients with Fractures
Early stabilization (within 24 hours) of long bone fractures, particularly of the tibia and femur, is said to be vital in the prevention of FES, as it allows patients to: [31] [32] −
Mobilize more quickly
- Decrease the incidence of ARDS and pneumonia
- Reduce the length of hospital stay.
Strategies for early stabilization of Fractures
- Early fixation of long bone fracture to stabilize, prevent or decrease the severity of FES [33]
- External fixation with plate and screw reduces the risk of emboli formation than Intramedullary nailing [34]
- Preoperative use of methylprednisolone may prevent the occurrence of FES [23]
- Continuous hemodynamic monitoring, O2 saturation
- Initiation of O2 supplementation and supportive care.
What is the prognosis of FES?
- Delayed diagnoses and lack of immediate supportive care lead to poor prognosis
- Acute fulminant FES may lead to death due to right heart failure.
- ARDS is said to be the leading cause of death in patients with FES.
- Other factors like increased age, multiple underlying medical problems, co-morbidities and/or decreased physiologic reserves have worse outcomes.[35]
References
- Michael E. K and Mark J. S. Fat embolism syndrome. Int J Crit Illn Inj Sci. 2013 Jan-Mar;
3(1): 64–68.doi: 10.4103/2229-5151.109426 - Nissar S. Emergency management of fat embolism syndrome. J Emerg Trauma Shock.
2009 Jan-Apr; 2(1): 29–33. doi: 10.4103/0974-2700.44680 - Von Bergmann E. Ein fall todlicher fettenbolic. Berl Klin Wochenscher. 1873;10:385. 3 4.
White T, Petrisor BA, Bhandari M. Prevention of fat embolism syndrome. Injury. 2006;
37S:S59–67. - Stein PD, Yaekoub AY, Matta F, Kleerekoper M. Fat embolism syndrome. Am J Med Sci. 2008;
336:472–477. doi: 10.1097/MAJ.0b013e318172f5d2. - Gurd AR, Wilson RI. The fat embolism syndrome. J Bone Joint Surg Br. 1974;56B:408–16.
- Sarah M. Causes, Clinical Manifestations, and Treatment of Fat Embolism. Virtual Mentor.
2006;8(9):590-592. doi: - 10.1001/virtualmentor.2006.8.9.cprl1-0609.
- Malagari K,Economopoulo N, Stoupis C, Daniil Z, Papiris S, Müller NL, Kelekis D. High resolution CT findings in mild pulmonary fat embolism. Chest 2003; 123(4):1196-1201. doi:10.1378/chest.123.4.1196
- Kumar V, Fausto N, Abbas A. Robbins and Cotran’s Pathologic Basis of Disease. 7th ed. New York, NY: WB Saunders; 2005:137.
- Duis HJ. The Fat Embolism Syndrome. Injury. 1997;28:77–85.
- Shapiro MP, Hayes JA. Fat embolism in sickle cell disease: Report of a case with brief review of literature. Arch Intern Med. 1984;14:181–2.
- Dillerud E. Abdominoplasty combined with suction lipoplasty: A study of complications,revision and risk factors in 487 cases. Ann Plast Surg. 1990;25:333–8.
- Akhtar S. Fat embolism. Anesthesiol Clin. 2009;27:533-50, doi: 10.1016/j.anclin. 2009.07.018.
- Husebye EE, Lyberg T, Røise O. Bone marrow fat in the circulation: clinical entities and pathophysiological mechanisms. Injury. 2006 Oct;37 Suppl 4:S8-18. doi: 10.1016/j.injury.2006.08.036. Erratum in: Injury. 2007 Oct;38(10):1224.
- Nijsten MW, Hammer JP, Dius HJ, Posma JL. Fat embolism and patent foreamen ovale. Lancet. 1989;1:1271
- Sheikh N. Emergency management of fat embolism syndrome. Journal of Emergencies Trauma and Shock. 2009;2(1):29-33
- Bulger EM, Smith DG, Maier RV, Jurkovich GJ. Fat embolism syndrome, a 10-year review. Arch Surg 1997;132(4):435- 439. doi:10.1001/archsurg.1997.0143028010901
- Christie J,Robinson CM, Pell AC, McBirnie J, Burnett R. Transcardiac echocardiography during invasive intramedullary procedures. J Bone Joint Surg Br 1995 May; 77(3):450-5.
- Georgopoulos D, Bouros D. Fat embolism syndrome: clinical examination is still the preferable diagnostic method.Chest. 2003; 123:982–983.
- A Shaji, Drs, H C Rajpurohit, J A Shankar, A Saroch, M Bhatia, A K Pannu, Clinical triad of fat embolism syndrome, QJM: An International Journal of Medicine, Volume 115, Issue 2, February 2022, Pages 105–106, https://doi.org/10.1093/qjmed/hcab311,/li>
- Bulger EM, Smith DG, Maier RV, Jurkovich GJ. Fat embolism syndrome. A 10-year review. Arch Surg. 1997; 132:435–439.
- Lindeque BG, Schoeman HS, Dommissen GF, Boeyens MC, Vlok AL. Fat embolism syndrome: A double blind therapeutic study. J Bone Joint Surg Br. 1987;69:128–31
- Schonfeld SA, Ploysongsang Y, DiLisio R, Crissman JD, Miller E, Hammerschmidt DE, et al. Fat embolism prophylaxis with corticosteroid: A prospective study in high-risk patients. Ann Int Med. 1983;99:438–43.
- Capan LM, Miller SM, Patel KP. Fat embolism. Anesthesiol Clin North Am 1993;11:25-54.
- Gupta B, D’souza N, Sawhney C, Farooque K, Kumar A, Agrawal P, et al. Analysing fat embolism syndrome in trauma patients at AIIMS apex trauma centre, New Delhi India. J Emerg Trauma Shock 2011;4:337-41.,/li>
- Jain S, Mittal M, Kansal A, Singh Y, Kolar PR, Saigal R. Fat embolism syndrome. J Assoc Physicians India 2008;56:245-9.
- Ryu CW, Lee DH, Kim TK, Kim SJ, Kim HS, Lee JH, Choi CG, Suh DC. Cerebral fat embolism: diffusion-weighted magnetic resonance imaging findings. Acta Radiol. 2005; 46:528–533.
- Van den Brande FG, Hellemans S, De Schepper A, De Paep R, Op De Beeck B, De Raeve HR, et al. Post-traumatic severe fat embolism syndrome, with uncommon CT findings. Anaesth Intensive Care. 2006;34:102–6.
- Wong MV, Tsui HF, Young SH, Chan KM, Cheng JC. Continuous pulse oximeter, for in apparent hypoxemia after long bone fractures. J Trauma. 2004;56:356–62.
- Gabdullin, M. M., Mitrakova, N. N., Gatiatulin, R. G., Rozhentsov, A. A., Koptina, A. V., & Sergeev, R. V. (2012). Fat embolism syndrome. Sovremennye Tehnologii v Medicine, 2012(1), 108–114. https://doi.org/10.5005/jp/books/12787_20
- Bone LB, Johnson KD, Wiegelt J, Scheinberg R. Early versus delayed stabilization of femoral fractures. J Bone Joint Surg Am. 1989;71(3):336-340.
- Behrman SW, Fabian TC, Kudsk KA, Taylor JC. Improved outcome with femur fractures: early vs. delayed fixation. J Trauma. 1990;30(7):792-797.
- 33. Behrman SW, Fabian TC, Kudsk KA, Taylor JC. Improved outcome with femur fracture: Early VS delayed fixation. J Trauma. 1990;30:792–7.
- Wheelwright EF, Byrick RJ, Wigglesworth DF, Kay JC, Wong PY, Mullen JB, Waddell JP.Hypotension during cemented arthroplasty. Relationship to cardiac output and fat
embolism. J Bone Joint Surg Br. 1993 Sep;75(5):715-23. doi: 10.1302/0301-620X.75B5.8376426. - Nikolić S, Micić J, Savić S, Gajić M. Factors which could affect the severity of post-traumatic pulmonary fat embolism: A prospective histological study. Srp Arch Celok Lek.2003;131:244–8.