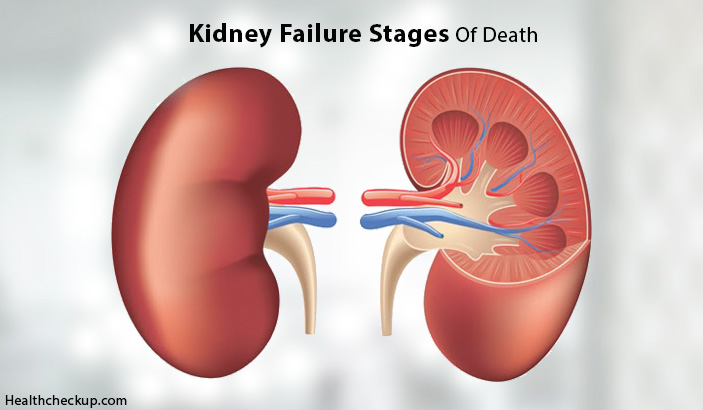
Our kidneys work day and night to filter our blood and get rid of all the toxic waste products in the form of urine. A lot of our body functions depend upon normal functioning of kidneys and the entire renal system.
Kidney failure is a serious clinical condition in which the kidneys fail to excrete metabolic end-products from the body. In this condition, the kidneys also fail to maintain fluid, electrolyte and pH balance of the blood.
Whenever a person is diagnosed with renal failure, the first question that comes into his/ her mind is that is it curable? And secondly, what are the stages of kidney failure causing death?
Renal Failure Types
Renal failure, both acute and chronic, can happen because of a wide variety of underlying causes such as systemic illnesses, metabolic or urological disorders or some renal pathology.
Acute Renal Failure
- Acute renal failure is a sudden but usually reversible loss of renal function. It is also called Acute Kidney Injury (AKI).
- There is a rapid decline in the functioning of kidneys.
- Deaths due to acute kidney injury range from 42-88%.
- It is commonly seen in old people and also as a complication of life-threatening conditions like trauma, sepsis, shock and urinary outflow obstruction.
Elderly people are prone to all kinds of renal failure due to reduced susceptibility and ageing. Some blood tests are suggested by doctors for kidney infection.
- When the kidney function fails, Glomerular Filtration Rate (GFR) reduces, which means that the kidneys are unable to remove nitrogenous waste substances from the body.
- Impaired functioning of kidneys also hampers the fluid, electrolyte and pH balance in the blood.
Types of Acute Renal Failure
| Type of Acute Renal Failure | Description |
|
Pre Tenal Failure
Occurs due to reduced blood flow to the kidneys.
It is the most common type of acute renal failure.
Treatment includes early identification of underlying cause and immediate correction of fluid loss. |
Causes 1. Blood loss or fluid loss as in
2. Anaphylactic shock (from sthe evere allergic reaction) 3. Septic shock (la ife-threatening condition from widespread infection which may cause organ failure) 4. Heart failure or cardiogenic shock 5. Reduced blood flow to kidneys due to drugs, vasodilators, ACE inhibitors, NSAIDs and radio-contrast agents used for diagnostic purposes. |
| Post Renal Failure
Occurs when there is an obstruction to the outflow of urine.
Treatment includes identification of the site of obstruction so that normal urine flow can be established before it damages the kidneys. |
Causes 1. Obstruction in both ureter
2. Obstruction in bladder outlet
3. Obstruction in urethra
|
| Intrinsic Renal or Intra Renal Failure
Occurs due to damage to structures of the kidneys.
Ischemic injury to tubules is reversible with treatment if detected early. Severe ischemia can cause irreversible changes.
|
Causes Acute Tubular Necrosis (destruction of renal tubules with the disturbed functioning of kidneys). It can be caused by 1. Reduced blood flow (ischemic necrosis)
2. Drugs and medications (Nephrotoxic)
3. Obstruction within tubules (intratubular)
4. Infections like acute glomerulonephritis and pyelonephritis. |
Course of Acute Renal Failure Can Be Divided into Three Phases for the Purpose of Understanding
|
Phase of Acute Renal Failure |
Description |
| Initiating phase or onset | Lasts for few hours or days until a tubular injury occurs. |
| Maintenance Phase | In this phase, GFR reduces resulting in
If untreated, hypertension develops neuromuscular symptoms like seizures, coma and death. |
| Recovery Phase | In this phase, renal tissue recovery takes place.
|
Early diagnosis and treatment of the underlying cause is the key to prevent deaths due to acute kidney failure. Fluid replacement is done to regulate fluid and electrolyte balance. Dialysis may also be required if the creatinine levels are too high.
Prognosis of acute renal failure is good if treatment is provided early, renal function improves rapidly without any renal impairment. In some cases where the treatment has been given late or when treatment has been ineffective, mild to moderate kidney damage may persist.
Know More About Improve Kidney Function To Avoid Dialysis
Chronic Renal Failure
- Chronic renal failure has a slow, insidious onset and usually develops over a period of years. It is also called as Chronic Kidney Disease (CKD)
- Unlike acute kidney injury, chronic renal failure is an irreversible deterioration of kidney function.
- Maximum number of patients progress to the final stages of chronic kidney failure resulting in death.
- Patients are asymptomatic and renal failure can be detected only by biochemical abnormalities. Due to excellent compensatory mechanisms in the body, impaired kidney function does not become evident at the very beginning.
- Progressive loss of kidney function leads to the appearance of signs and symptoms.
- When death is likely without renal replacement therapy, it is called End Stage Renal Disease/ Kidney Failure Stage of Death.
Causes For End-Stage Renal Disease
- Congenital and hereditary conditions like polycystic kidneys, Alport’s syndrome.
- Renal artery stenosis
- Hypertension
- Glomerular disease like IgA nephropathy
- Renal Interstitial Disease
- Systemic inflammatory diseases like SLE and vasculitis.
- Diabetes Mellitus
Stages of Progression of Chronic Renal Failure
|
Stage of progression |
Description |
| Diminished renal reserve |
|
| Renal Insufficiency
A protein-restricted diet is advised as the body has difficulty in removing end-products of protein metabolism, |
|
| Renal Failure |
|
| End Stage Renal Diseases
This is the final stage of kidney failure of death.
Dialysis or renal transplant is necessary for survival. |
|
Know More about Kidney Function Tests
Clinical Features of Chronic Kidney Failure
- Sodium and water imbalance result in hypertension. There is increased blood volume which can cause edema and cardiac failure.
- Potassium imbalance can cause cardiac arrhythmias.
- Impaired production of erythropoietin (a protein necessary for RBC formation) resulting in anemia. Anemia causes weakness, fatigue, insomnia, depression and in severe cases of cardiac failure.
- Impaired platelet function causes bleeding disorders and coagulation defect.
- Impaired pH balance causes metabolic acidosis.
- Impaired vitamin D and phosphate metabolism result in osteodystrophies (defective bone development).
It also causes hypocalcemia (reduced calcium in the blood) and hyper-parathyroidism.
Failure to Eliminate Nitrogenous Waste Results In
Cardiovascular Disorders – Left ventricular hypertrophy, pericarditis, and hypertension.
Gastro-Intestinal Tract (GIT) Disorders – Nausea, vomiting, anorexia, metallic taste in mouth, hiccups and bleeding and ulceration of GIT mucosa.
Neurological Disorders – Peripheral neuropathy, restless leg syndrome, burning sensation of feet as a feature of uremia. In severe cases, uremic encephalopathy may occur with features of seizures, delirium and comas.
Skin Disorders – Pallor, bruising, skin dryness and itching from high serum phosphate levels. Nails become thin and brittle with a dark band followed by a light band at the edge. This is called Terry’s nails.
Sexual Dysfunction – From high levels of urea and neuropathy. Impotence and loss of libido in males. In women, infertility and menstrual abnormalities are seen.
The rate by which kidney function deteriorates is different for different patients. To treat CKD effectively, identifying the underlying cause is important. Identify reversible factors which make renal function worse like diet, medications and renal outflow obstruction and treat accordingly.
In final kidney failure stages of death, medications and measures are taken to prevent further damage of kidneys and to limit adverse reactions of kidney failure on the body. Dialysis and transplant are suggested when there are severe uremia and electrolyte imbalance.
Dr. Himanshi is a Homoeopathic consultant and currently working as a lecturer in Post-graduate faculty of Homeopathy, Parul University, Vadodara. Completed BHMS and MD in Homeopathy in January 2018 and also has a clinical experience of about 6 years. Personal interests include reading, spending time with family and traveling.