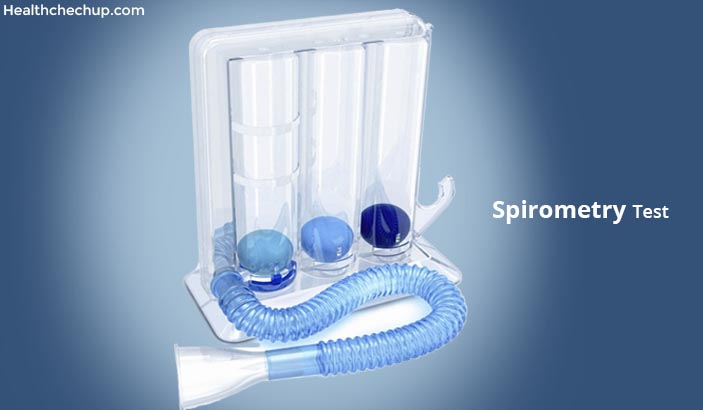
What Is Spirometry?
Spirometry is also called a pulmonary function test. The device used to carry out the test is called a Spirometer or a Flow Meter.
It is a means to assess the integrated mechanical functioning of the lungs, respiratory muscles, and chest wall. This is done by measuring the total volume of air exhaled (Total Lung Capacity – TLC) to maximal expiration (Residual Volume – RV).
When To Do A Spirometry Test?
It is a valuable diagnostic and prognostic tool that can be used for the following purposes
- Early detection of airflow obstruction.
- Diagnosis of respiratory disorders in patients by evaluating results. The pattern of volume loop created points to the type of respiratory disorder but not the exact disease.
- Monitoring patient’s response to the treatment and course of respiratory illness.
- A guide to the further course of treatment and medical intervention.
- Investigation of non-respiratory diseases which may impact lung function.
Example: Connective tissue disorders and neuromuscular diseases. - Screening or evaluation of persons at high risk for respiratory diseases
Example: Environmental or occupational exposure to radiation, asbestos, silica - Preoperative risk evaluation prior to lung resection and cardiothoracic surgeries.
- Following lung transplant to detect signs of acute rejection, infection and obliterative bronchiolitis (chronic organ rejection).
- Evaluation of respiratory status before strenuous physical activity.
- Spirometry should ideally be performed regularly in persons above the age of 35 years with a history of cigarette smoking.
- Spirometry can effectively differentiate between psychosomatic and organic respiratory disorders.
- Spirometry can be performed in acute respiratory infections such as tuberculosis only if the risk of cross-contamination becomes negligible.
[Read – Immediate Effects of Smoking]
Persistence Of The Following Signs And Symptoms Are An Indication For A Spirometry Test
- A cough
- Wheezing or crackles
- Breathlessness or shortness of breath
- Abnormal chest x-ray
How To Do A Spirometry Test?
- The spirometry test is a relatively simple and quick procedure.
- It is to be performed in a sitting position with head slightly elevated or slightly leaned back.
- The nurse or technician will place the mouthpiece of the spirometer.
- The patient is asked to inhale rapidly and completely followed by forceful exhalation for as rapidly and as long as possible.
- Patients should not lean forward during the test.
- The patient should exhale for at least 6 seconds.
- This forceful inhalation and exhalation may have to be repeated for up to 4-5 times (maximum 8 number of times).
Spirometry Test Preparation
Patients Are Supposed To Observe The Below-Mentioned Guidelines Before A Spirometry Test As They Can Impact Test Results
- Patients are advised to not smoke at least an hour prior to the test.
- Patients reporting for the test should ensure that they do not eat a large meal at least 2 hours prior to the test.
- Patients should not consume alcohol at least 4 hours before reporting for the test.
- Patients should avoid vigorous exercises at least an hour before the test.
- Adequate care should be taken to avoid tight clothing when going for the test.
- Patients using false teeth can use it during the test unless it interferes while performing the test.
- Patients are usually explained about the test.
- Height and weight are measured before beginning the test.
Some Patients May Experience The Following Signs And Symptoms Due to Repeating The Test
- Lightheadedness or dizziness
- A headache
- Fainting
- Transient urinary incontinence
Spirometry Test Results And Interpretation
Interpretation of spirometry test results depends entirely upon the test quality and how effectively it is performed by patients. A test which fails to meet the standard guidelines can yield unreliable results. The American Thoracic Society has laid down few guidelines for an acceptable spirometry test which includes
- Should start from full inflation
- Shows minimal hesitation at the start of forced expiration
- Shows an explosive start of the forced expiration
- Shows no evidence of a cough in the first second of forced expiration.
- There is no leak at the mouth
- No spirometry or test result can be rejected solely on the basis of poor repeatability.
- Meets one of the following three criteria that define a valid end-of-test (EOT criteria):
➢ The patient cannot or should not continue further exhalation. Patients can terminate expiration if they experience discomfort.
➢ The volume-time curve shows no change for more than 1 second and the person has tried to exhale for >/= 3 seconds or more in children less than 10 years of age and for >/= 6 seconds for patients above the age of 10 years.
➢ If the test fails to exhibit an expiratory plateau.
A final test report is generated for evaluation if the test meets the above-mentioned test quality parameters.
Spirometry Results Are Expressed As Graph Of Measure Of Volume Against Time. The First Graph Can Be Interpreted As Follows
- Forced Vital Capacity (FVC) – The volume of air that can be exhaled forcefully after maximal inhalation.FVC is less than 3 seconds in normal people.FVC is prolonged in patients with obstructive lung diseases.
- FEV1 – The volume of air exhaled in the first second of FVC.Normal persons can exhale up to 75 – 80% of FVC during the first second.The ration of FEV1/FVC helps to determine the type of lung disease.
- Forced Expiratory Flow (FEF) – Flow of air coming out of the lungs during the middle portion of forced expiration.FEF can be 25 – 75% in normal persons (FEF25-75%).A second graph is called the volume loop. In a volume loop, the part of the curve below baseline indicates inspiration and the curve above baseline indicates expiration.
This Graph Can Be Interpreted As Follows
- Peak Expiratory Flow (PEF) – It is the speed during maximal forced expiration after complete inhalation.
PEF is measured in liter per second. PEF of a normal person is 80 – 100%. - Tidal Volume (TV) – It is the amount of air inhaled and exhaled during normal breathing.
Dr. Himanshi is a Homoeopathic consultant and currently working as a lecturer in Post-graduate faculty of Homeopathy, Parul University, Vadodara. Completed BHMS and MD in Homeopathy in January 2018 and also has a clinical experience of about 6 years. Personal interests include reading, spending time with family and traveling.