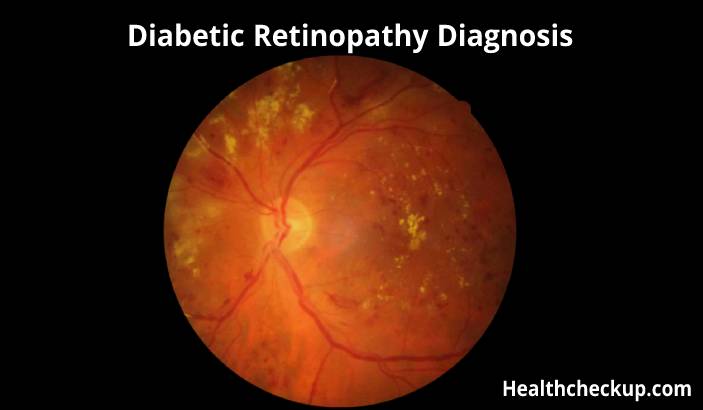
Diabetic retinopathy is a serious complication of diabetes that can lead to blindness if left untreated. It occurs when high blood sugar levels damage the blood vessels in the retina, the light-sensitive part of the eye. In this article, we will discuss the diagnosis of diabetic retinopathy, including when to see a doctor, tests to diagnose the condition, and treatment options.
When to see a doctor:
It is important for people with diabetes to have regular eye exams to screen for diabetic retinopathy. The American Diabetes Association recommends that people with type 1 diabetes should have their first eye exam within 5 years of diagnosis, and people with type 2 diabetes should have their first eye exam at the time of diagnosis. After the initial exam, people with diabetes should have a comprehensive dilated eye exam at least once a year.
In addition to regular eye exams, people with diabetes should see a doctor if they experience any of the following symptoms:
- Blurred vision
- Floaters or spots in their vision
- Dark or empty spots in their vision
- Poor night vision
- Colors appearing faded or washed out
Tests to diagnose Diabetic Retinopathy:
During a comprehensive dilated eye exam, the eye doctor will use special eye drops to dilate the pupil and examine the retina for signs of diabetic retinopathy. In some cases, the doctor also uses a special camera to take pictures of the retina.
In addition to a dilated eye exam, other tests are used to diagnose diabetic retinopathy, including:
- Fluorescein angiography: This test uses a special dye to highlight the blood vessels in the retina. The dye is injected into a vein in the arm, and pictures are taken as the dye circulates through the retina.
- Optical coherence tomography (OCT): This test uses light waves to create detailed images of the retina. It can help detect swelling or fluid buildup in the retina, which are signs of diabetic retinopathy.
Treatment options for Diabetic Retinopathy:
The treatment for diabetic retinopathy depends on the severity of the condition. In the early stages, the best treatment is to control blood sugar levels, blood pressure, and cholesterol to prevent further damage to the blood vessels in the retina.
In more advanced cases, treatment options include:
- Laser treatment: This involves using a laser to seal off leaking blood vessels and to shrink abnormal blood vessels in the retina.
- Vitrectomy: This is a surgical procedure that involves removing the vitreous gel and any blood that has leaked into the eye. The gel is replaced with a saline solution.
In addition to these treatments, there are several lifestyle changes that people with diabetes can make to help prevent diabetic retinopathy from worsening. These include:
- Controlling blood sugar levels
- Controlling blood pressure
- Maintaining a healthy weight
- Exercising regularly
- Not smoking
In conclusion, diabetic retinopathy is a serious complication of diabetes that can lead to blindness if left untreated. Regular eye exams are important for people with diabetes to screen for this condition. If you experience any symptoms of diabetic retinopathy, you should see a doctor right away. Tests to diagnose diabetic retinopathy include a dilated eye exam, fluorescein angiography, and OCT. Treatment options depend on the severity of the condition and includes laser treatment or vitrectomy. In addition to medical treatments, lifestyle changes can help prevent diabetic retinopathy from worsening.