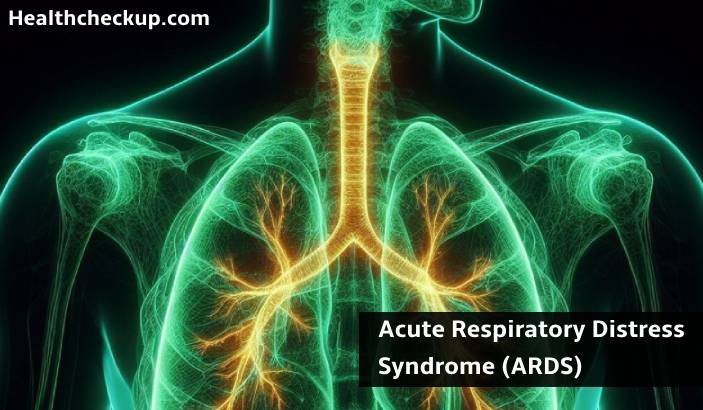
Acute Respiratory Distress Syndrome (ARDS) is a severe and life-threatening condition characterized by rapid onset of widespread inflammation in the lungs. This condition leads to impaired gas exchange, resulting in severe respiratory failure.
What is ARDS?
ARDS is a type of respiratory failure that occurs when fluid builds up in the alveoli, the tiny air sacs in the lungs. This fluid accumulation prevents oxygen from properly entering the bloodstream, leading to severe shortness of breath and hypoxemia (low blood oxygen levels). ARDS typically develops in response to a variety of underlying conditions that cause direct or indirect lung injury.
Causes of ARDS
ARDS can be triggered by numerous conditions and events, broadly categorized into direct and indirect lung injuries.
Direct Lung Injury
- Pneumonia: Severe bacterial, viral, or fungal infections of the lungs can cause ARDS.
- Aspiration: Inhalation of gastric contents, food, or other substances into the lungs can lead to inflammation and ARDS.
- Inhalation Injury: Exposure to toxic smoke, chemicals, or other harmful substances can directly damage the lung tissues, resulting in ARDS.
- Near Drowning: Inhalation of water during near-drowning incidents can cause significant lung injury and ARDS.
Indirect Lung Injury
- Sepsis: A widespread infection in the body that leads to systemic inflammation and can result in ARDS.
- Severe Trauma: Major injuries, including fractures and burns, can trigger systemic inflammatory responses that affect the lungs.
- Pancreatitis: Inflammation of the pancreas can release inflammatory mediators that harm the lungs, leading to ARDS.
- Blood Transfusions: Multiple blood transfusions can cause transfusion-related acute lung injury (TRALI), a form of ARDS.
- Drug Overdose: Certain drugs, including opioids and sedatives, can depress respiratory function and lead to ARDS.
Symptoms of ARDS
The symptoms of ARDS usually appear within hours to a few days after the initial injury or infection. Key symptoms include:
- Severe Shortness of Breath: Patients often experience extreme difficulty breathing, which can worsen rapidly.
- Rapid Breathing: Increased respiratory rate as the body attempts to compensate for low oxygen levels.
- Hypoxemia: Critically low levels of oxygen in the blood, leading to cyanosis (bluish discoloration of the lips and skin).
- Cough: A persistent cough that produce frothy sputum.
- Fatigue and Weakness: Generalized fatigue and weakness due to inadequate oxygen supply to the muscles and organs.
- Confusion: Reduced oxygen levels can affect brain function, leading to confusion, agitation, or lethargy.
Diagnosis of ARDS
Diagnosing ARDS involves a combination of clinical evaluation, imaging studies, and laboratory tests. The following steps are typically involved:
- Clinical Assessment: A thorough assessment of symptoms, medical history, and potential risk factors is conducted.
- Chest X-ray: A chest X-ray can reveal diffuse infiltrates, indicating fluid accumulation and inflammation in the lungs.
- CT Scan: A more detailed imaging study that provides a clearer picture of lung abnormalities.
- Blood Tests: Arterial blood gas (ABG) analysis measures oxygen and carbon dioxide levels in the blood, helping to assess the severity of hypoxemia.
- Pulmonary Function Tests: These tests evaluate lung capacity and function, helping to determine the extent of respiratory impairment.
Treatment of ARDS
ARDS is a medical emergency that requires prompt and intensive treatment. The primary goals of treatment are to improve oxygenation, support lung function, and address the underlying cause of the condition. Treatment strategies include:
Mechanical Ventilation
Mechanical ventilation is the cornerstone of ARDS treatment. It involves using a machine to assist or fully control a patient’s breathing. Key aspects of mechanical ventilation in ARDS include:
- Low Tidal Volume Ventilation: Using smaller breaths to reduce lung injury caused by over-distension.
- Positive End-Expiratory Pressure (PEEP): Applying pressure at the end of expiration to keep the alveoli open and improve oxygenation.
- Prone Positioning: Placing the patient on their stomach can improve oxygenation by redistributing blood flow and air in the lungs.
Oxygen Therapy
Supplemental oxygen is provided to maintain adequate blood oxygen levels. In severe cases, extracorporeal membrane oxygenation (ECMO) is used. ECMO is a specialized form of life support that uses a machine to oxygenate the blood outside the body, allowing the lungs to rest and heal.
Fluid Management
Careful management of fluid balance is crucial in ARDS. Too much fluid can worsen lung edema, while too little can lead to low blood pressure and organ failure. Diuretics are used to remove excess fluid from the body.
Medications
- Antibiotics: If an infection is the underlying cause, antibiotics are administered to treat the infection.
- Anti-inflammatory Medications: Corticosteroids can be used to reduce inflammation in the lungs, although their use is controversial and must be carefully considered.
- Sedatives and Pain Relief: Sedatives and pain relievers are administered to improve comfort and reduce anxiety, especially during mechanical ventilation.
Complications of ARDS
ARDS can lead to various complications, some of which can be life-threatening:
- Lung Scarring: Persistent inflammation can lead to fibrosis, causing long-term damage and reduced lung function.
- Organ Failure: Severe hypoxemia can impair the function of vital organs such as the heart, kidneys, and liver.
- Blood Clots: Immobility and inflammation can increase the risk of blood clots, leading to deep vein thrombosis (DVT) or pulmonary embolism (PE).
- Infections: Prolonged use of mechanical ventilation and invasive procedures increase the risk of secondary infections.
Prognosis and Long-Term Outlook
The prognosis for ARDS varies depending on the severity of the condition, the patient’s overall health, and the underlying cause. The mortality rate for ARDS is high, ranging from 30% to 50%, but advances in critical care have improved outcomes.
Survivors of ARDS experience long-term effects, including:
- Reduced Lung Function: Many patients recover fully, but some have persistent respiratory issues and reduced exercise capacity.
- Physical Weakness: Prolonged hospitalization and immobility can lead to muscle weakness and reduced physical strength.
- Psychological Impact: Survivors experience post-traumatic stress disorder (PTSD), anxiety, and depression.
Summing Up
Acute Respiratory Distress Syndrome (ARDS) is a severe and life-threatening condition that requires immediate medical attention. Understanding the causes, symptoms, diagnosis, and treatment options for ARDS is essential for managing this complex condition and improving patient outcomes. With prompt and appropriate treatment, many patients can recover from ARDS, although some experience long-term effects. Ongoing research and advances in critical care continue to improve the understanding and management of ARDS, offering hope for better outcomes for those affected by this challenging condition.
I specialize in writing about health, medical conditions, and healthcare, drawing extensively from scientific research. Over the course of my career, I have published widely on topics related to health, medicine, and education. My work has appeared in leading blogs and editorial columns.